Lethal heat and climate justice.
The increase in extreme heat events around the world shows that the impact of climate change is increasingly lethal. Any climate justice strategy needs to include ‘heat justice’ and a politics of resilience.
More than 5 million people die every year globally because of excessive heat or cold, and heat-related deaths are on the rise. 9.4% of global deaths per year are attributable to heat or cold exposure. Heat is a major killer worldwide, but many heat-related deaths are preventable.
When people are exposed to extreme heat, they can suffer from fatal heat exhaustion or heat stroke. Heat can also contribute to deaths from heart attacks, strokes and other cardiovascular conditions. Children, adults over 65 and people with cardiovascular and respiratory illnesses have a higher than average risk of heat-related death and the poorest are the most vulnerable.
The impacts of both heat and cold are greatest in more deprived areas, and understanding these patterns should inform public health policies and adaptation strategies at local and national levels and protect the most vulnerable groups.
“It was getting hotter.” (Fiction)
These are the opening words of the first chapter of Kim Stanley Robinson’s ‘The Ministry of the Future’ – one of the most powerful passages of climate fiction ever written. The novel offers a vision of a near-future where climate change is having lethal impacts on a massive scale. Published in 2020, it hardly qualifies as ‘speculative’ fiction since the type of extreme heat events it describes have already been experienced in many parts of the world and will only get worse.
One of the central characters, Frank May from Jacksonville, Florida, is working for an aid charity in its clinic in an ordinary town in the Indian state of Uttar Pradesh. He witnesses the devastating human consequences of extreme heat and high humidity combined with power outages.
The air in the coolest part of the day reminds him of a sauna. The monsoon has not yet come and at 6am it is already 38 degrees. With the dawn come wails of dismay from neighbouring rooftops as people discover that other sleepers on their roof are not waking up. As the power goes down and illegal diesel and kerosene are fired up, the air, already bad, becomes a blanket of exhaust.
Venturing out, Frank finds that:
“Every building has a clutch of desperate mourners in its entryway… As with coughing, it was too hot to wail very much. It felt dangerous even to talk, one would overheat. And what was there to say anyway? It was too hot to think.”
People approach Frank for help and he suggests they go to the lake.
“The water will keep you more cool”
But a man responds:
“That water is in the sun. It’s as hot as a bath. It’s worse than the air.”
His organisation’s headquarters in Delhi can’t send help as power is out there, and across Uttar Pradesh too. The only hope is that the heatwave might end soon as rising air over the land pulls in cooler air off the ocean.
When Frank himself makes his way to the lake in the late afternoon, he finds a desperate scene: people’s heads dotting the surface of the water all around the shores and not all of them alive. After sunset, like everyone else, he gets into the water.
“Hot water in one’s stomach meant that there was no refuge anywhere, the world both inside and outside well higher than human body temperature ought to be. They were being poached… All the children were dead, all the old people were dead…Everyone was dead.”
‘What it’s like to live through India’s nonstop heat wave’ (Reality)
The reality is hardly less shocking, in this account from the Bloomberg website by Archana Chaudhary and Akshat Rathi of a single day in New Delhi when the city of 19 million struggled to cope with killer temperatures (May 2022)
“While New Delhi’s growing middle class may have access to air-conditioned offices, shopping malls and cars, there are millions of migrant workers who make up 40% of its population that have spent these extreme days without any access to relief. Even for those who can afford cooling devices, the threat of blackouts from surging power demand remains a constant worry.”
Early in the morning, Darshan Mukhiya, a vegetable vendor, wheels his 83-year-old father in a cart to update his health records at a government office two miles away and avoid losing access to benefits. They set out before it’s too hot to be in the open… at home the only option for cooling off is to soak in the polluted river.
Mahato, 51, helps to run a school in the shade of a nearby bridge.
Metro trains roll by overhead. The air-conditioned carriages packed with people who might otherwise walk or cycle. There should be 300 students, but many families have left the city’s oppressive heat for the villages. The 50 children are drenched in sweat, making frequent trips to the only drinking water tap available. They shut down the school when it goes above 45°C, which doesn’t normally happen until late May or June. Many children who live in cramped homes have been suffering from upset stomachs and even fever, he says, with cases of malaria on the rise as mosquitoes breed in the heat and humidity.
By 1 p.m. it’s 43°C.
Bhumi, 18, shares an eight by ten-foot room with a single window in a shantytown in southern Delhi with her five siblings and their parents. They cook and sleep out on the cramped terrace where it’s slightly cooler. The single fan isn’t much help, she says, and the power could go out at any moment. Her neighbourhood has experienced at least two cuts every day.
Madhu has just heard that government tankers meant to deliver water to her slum in southwestern Delhi have been cancelled. The settlement hasn’t been recognized by the authorities and there’s no tap water available.
“The heat has left us to the mercy of the water mafia,” she says, referring to private dealers who charge between 100 and 200 rupees per 20-liter jerrycan… Madhu and her neighbours will have to spend hours standing in long lines the next day to secure extra water. It also means lost work hours and forcing children to skip school to make sure their families get enough to drink.
By the evening, lingering heat combined with high humidity levels can prevent the body from sweating enough to cool down. That’s often when people can suffer fatal heat strokes. With dense residential clusters and even denser slums, Indian cities are particularly vulnerable to the urban island heat effect.
To make things worse, the increasing number of cooling devices are transferring heat from buildings to the outside spaces, making it harder for the city to cool down despite its abundant greenery.
Vandana, 47, a social activist in south Delhi, says the heat in her low-income residential complex has become unbearable as more and more air-conditioners whirr.
What about the UK?
Compared to India, the UK has had fewer and less extreme heat events, with less severe human consequences. Apart from anything else, the UK is much richer, with twenty times more GDP per capita. But what both countries have in common is the unequal impact of heatwaves on their people.
In the UK, we have just experienced a short and uncomfortable heat wave and we know that climate change means that such events will become more frequent and intense, causing preventable deaths. The August 2003 European heatwave led to the heat-related deaths of around 70,000 across Europe, including over 2,000 in the UK. Heat-related risks are greater in urban areas and London has the highest heat-related mortality rate, with 3.21 excess deaths per 100,000 people, which translates to 170 heat-related excess deaths each year.
England does have a Heatwave Plan, but it is demonstrably inadequate, and a Department of Health review of arrangements for managing heatwave risks concluded that “there is no definitive evidence” that the plan has been effective. The Government had not made significant improvements in recent years and last summer, there were 1,634 excess deaths during periods of heatwave conditions, and the figure for summer 2020 was even higher at 2,556. The slow pace of action means that the UK is likely to experience hundreds of preventable deaths this year. More could be done to mitigate the risk. The Climate Change Act requires us to have a National Adaptation Programme and we need a National Heat Risk Strategy to improve the response to heatwaves.
A politics of comfort and resilience
A heatwave, like a pandemic or an economic crisis, reveals and magnifies inequality. Like food, shelter and safety, physical comfort is essential for human life. To be comfortable, we need to be within a range of bearable temperatures, which may differ from the natural ones around us. We need this basic level of comfort to be able to work, rest, think, learn and care for others. If we are in discomfort, we are unable to thrive, contribute, participate, earn or learn.
In order to achieve comfort, we need shelter, shade, heating and cooling systems. The social provision of comfort, as part of an infrastructure of resilience, is often very basic or non-existent, while access to private comfort is wealth dependent. Our natural and built environments can be designed for comfort, but being wealthy buys us better access to comfort and therefore greater enjoyment of life and everything society has to offer. Resilience has to be paid for and access to it is not universally available. If we can afford shelter, shade, air conditioning, ventilation, and the conditions of comfort, we can be ‘resilient’ and get more from life.
If physical comfort is treated a commodity, it will be unequally distributed – like all market commodities. If we can’t afford it, we won’t have access to it. Being poor often means being excluded from the opportunity to be resilient, from access to comfort and all its benefits, and this leads to discomfort of many kinds; personal and social. The inequality of comfort goes on to magnify other inequalities.
A decent level of physical comfort should be a universal human right, and it should be equitably distributed. Every heatwave should serve to remind us that climate justice is a political issue.
See also:
‘The Ministry of the Future’ by Kim Stanley Robinson (December 2020)
Education, social justice and survival in a time of crisis (July 2022)
Nancy Fraser’s eco-socialist common-sense (August 2022)
Owning our crises (March 2022)
Extreme temperatures could kill 5 million people a year. The Guardian (08/07/22)


 In the essay ‘
In the essay ‘



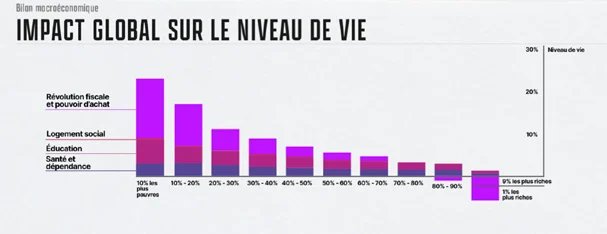
 2022 is a big election year in France, with the presidential election in April followed by the parliamentary (National Assembly) elections in June. Each of these elections has two rounds, meaning that most voters can expect to go to the polls on four separate occasions this Spring.
2022 is a big election year in France, with the presidential election in April followed by the parliamentary (National Assembly) elections in June. Each of these elections has two rounds, meaning that most voters can expect to go to the polls on four separate occasions this Spring.

 We are trashing our home planet, people are suffering and dying from avoidable causes, systemic inequalities are widening, injustice, exploitation and conflict of all sorts proliferate and we continue to make choices we know are unsustainable. The consequences of our failures are more evident than ever but it feels like we haven’t fully developed the ideas, the dialogue and the politics to deal with the situation in we find ourselves. We may just be coming to a collective realisation that our current ways of doing things will not get us out of this and that there needs to be sustained structural change.
We are trashing our home planet, people are suffering and dying from avoidable causes, systemic inequalities are widening, injustice, exploitation and conflict of all sorts proliferate and we continue to make choices we know are unsustainable. The consequences of our failures are more evident than ever but it feels like we haven’t fully developed the ideas, the dialogue and the politics to deal with the situation in we find ourselves. We may just be coming to a collective realisation that our current ways of doing things will not get us out of this and that there needs to be sustained structural change.


 Bewilderment is an entirely rational response to what we are collectively doing to our planet. Confronted by the injustices, dysfunction and unsustainability of the world we’ve created, how can we not react with bewilderment?
Bewilderment is an entirely rational response to what we are collectively doing to our planet. Confronted by the injustices, dysfunction and unsustainability of the world we’ve created, how can we not react with bewilderment?